Veterinary Emergency and Referral Hospital of West Toronto

Hours of Operation
Emergency Hours
24 Hours

Surgery Hours
Monday - Thursday 9:00am - 6:00pm
Friday, Saturday, Sunday, and HOLIDAYS CLOSED

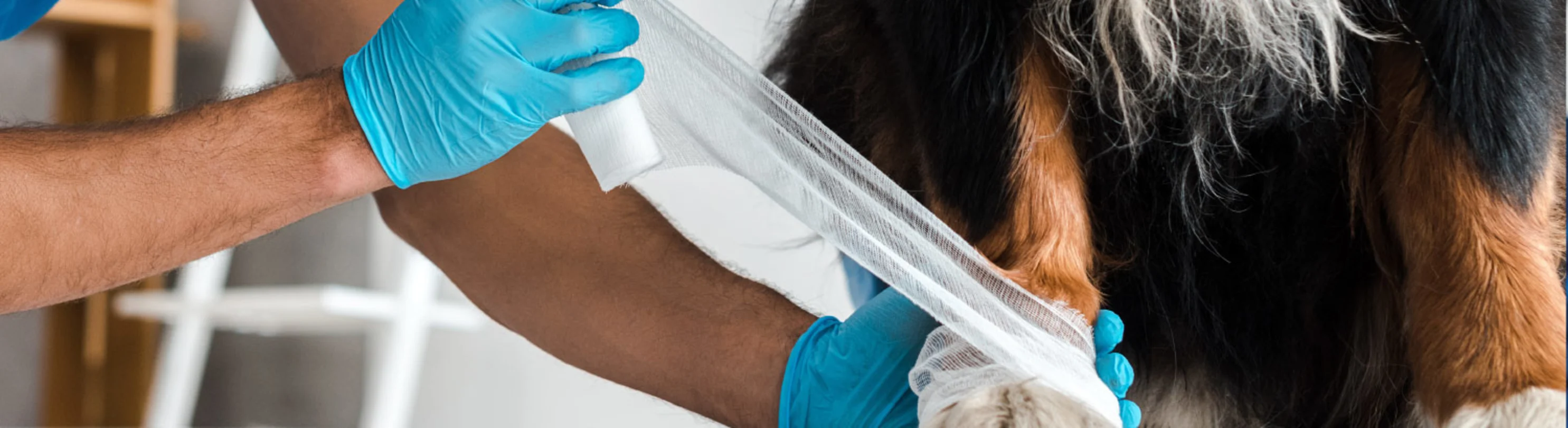
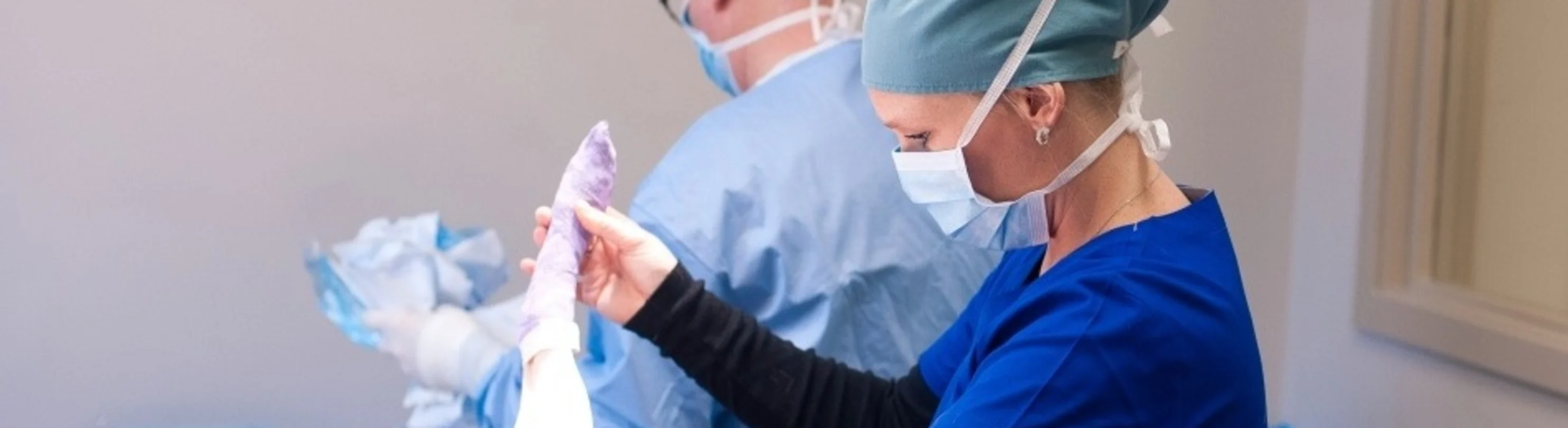
Is Your Pet Experiencing an Emergency?
What to Expect When Visiting Our Veterinary Emergency and Referral Hospital
All pets are seen on a walk-in basis, your pet will be triaged upon arrival and priority given to those more critical. We understand that these situations can be stressful and have a strict policy in place ensuring that you understand why we advise certain diagnostics and treatments. Our staff strive on being teachers and will be there with you every step of the way.